Your views

Your feedback is vital to us as we continue to increase the quality of our services.
You are here:
Date: 22 February 2025
Time: 11:54
Implant types
- Middle ear implant (MEI)
- Cochlear implant (CI)
- Electro-acoustic stimulation (EAS) implant
- Auditory brainstem implant (ABI)
Middle ear implant (MEI)
There are different types of middle ear implant but their function is the same: to assist in the mechanical transmission of sound waves to the inner ear (cochlea). The MEI is inserted into the middle ear and either attaches onto one of the middle ear bones or to the round window between the middle ear and the cochlea.
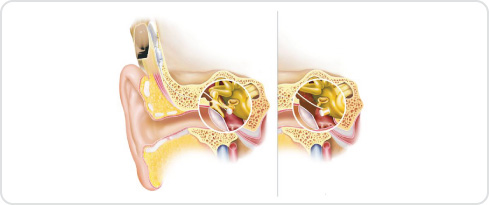
The attachment enhances the transmission of the sound waves to the cochlea. A MEI is inserted during a 2-3 hour operation under a general anaesthetic. A MEI is only appropriate for someone who has already tried conventional hearing aids in the past and who has significant clinical reasons that contra-indicate continued hearing aid use.
Some systems are totally implantable and there is nothing to wear on the outside. Other systems require the person to wear a small button receiver held magnetically behind the ear. The team will recommend the device that is most appropriate for each patient.

Cochlear implant (CI)
A cochlear implant (CI) may be recommended for someone who has severe to profound permanent deafness in both ears but who has either had better hearing in the past or who has always used the hearing they have left through conventional hearing aids.
The CI system has two parts.
The internal electrode array
The internal electrode array is inserted into the organ of hearing (cochlea) by a specialist ENT consultant. The operation is performed under a general anaesthetic and normally takes about two to three hours. First, a small area of hair is shaved from behind the ear and then a hollow is created in the bone behind the ear, under the skin. The electronics and magnet of the implant are fixed here. The surgeon then inserts the electrode array into the cavity of the cochlea itself. The electrodes are placed so that they stimulate the hearing nerve endings. Once all the components are in place, the area is stitched up and a dressing applied.
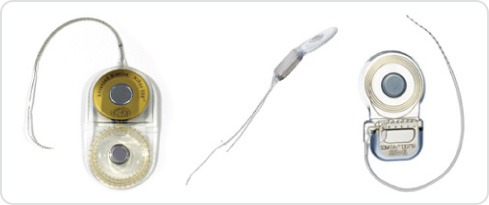
Most people only spend a day or two in hospital after surgery and many can return to work after a short period of recovery. Some patients report some dizziness following surgery but this is treatable and usually subsides after a short while. Afterwards, all that is visible on the outside is a scar behind the ear. You may be able to feel a slight bump under the skin; this is the internal electronics and magnet of the implant.
Remember, you will not be able to hear on this side until the implant is activated. This is called the switch-on, and takes place approximately three to four weeks later. We try and preserve the natural hearing in the ear using “soft” surgical techniques, but this cannot be guaranteed. If you were a hearing aid user, you can continue to use your hearing aid on the non-implanted ear. Some people find this a difficult period, especially if they have received the implant in their "good" ear. Interim appointments with the hearing therapist can be arranged prior to switch-on, if extra support is needed during this time.
The internal components of the cochlear implant cannot work without the external parts, which are fitted approximately three to four weeks after the operation, in order to give the ear time to heal. The fitting appointments are called your switch-on.
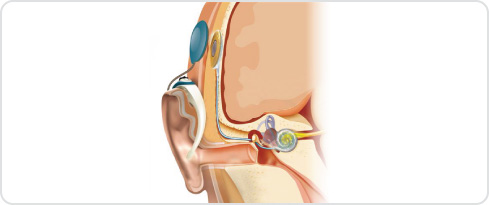
External parts
The external components consist of several parts, including a microphone, which picks up sounds in the environment. These sounds are then encoded by the speech processor, which looks like a large hearing aid but in fact is more like a specialised computer. The encoded signals are passed across the skin via a magnetic connection to the internal components.
This magnetic connection is made via the coil or headpiece, which is a small round device on the side of the head. It transmits the encoded signals to the internal device via radio waves and is held in place over the internal electronics by a magnet.
The signals are then decoded and the internal electrodes are activated in a particular sequence in order to produce a sensation of sound.
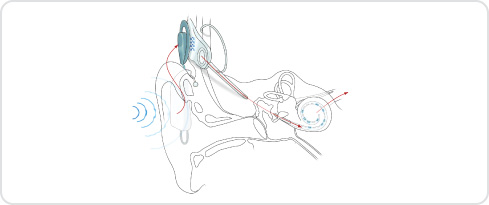
There are several different manufacturers of cochlear implant systems. Whilst each system has its own features and advantages, all work in a similar way. All the cochlear implant systems currently used on our programme use a behind-the-ear (BTE) speech processor with a magnetic headpiece. All new patients will receive a BTE system, unless there are particular clinical reasons for selecting a body worn processor.

A cochlear implant cannot restore normal hearing. It will, however, give a perception of hearing to people who previously received limited benefit from high-powered hearing aids. The sounds generated by the implant are electrical in origin and some people report that at first, the implant sounds electronic and unnatural.
During the Switch-on period, some people find it hard to understand and distinguish these new sounds. However, with support from the Implant Team, patients learn to make sense of the signals and gradually, over time, the sounds become more pleasant, natural and meaningful.
The vast majority of our patients report benefit from their implants, although the amount of benefit varies from person to person and depends on a variety of factors.
Most people are able to hear a wide range of environmental sounds. Many understand familiar phrases without lip-reading and some patients find they are able to use the telephone again. The Team will discuss with you the type of benefits you might expect to gain from your implant, based on your individual circumstances.
Where possible, we encourage our patients to continue to use their conventional hearing aid on the other ear, in conjunction with the CI. This is known as bimodal hearing.
Electro-acoustic stimulation (EAS) implant
The EAS implant has some of the same components of a cochlear implant. The difference is that the electrode array only stimulates the region in the cochlea that processes high pitched sounds. It does not stimulate the low pitched region, leaving the natural hearing for low pitches potentially undamaged. The EAS device has a hearing aid component built in for conventional amplification of the low pitched sounds. It should be noted that whist the goal is to preserve the remaining hearing, the inner ear structures are highly delicate and sensitive and so some reduction of natural hearing may occur after surgery.
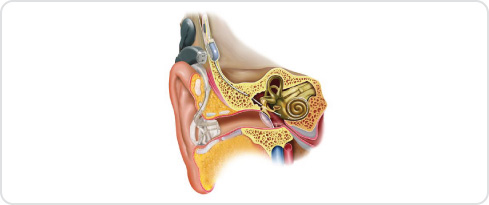
Following switch-on the patient will hear the high pitched sounds electronically through the implant. Low to mid pitches are amplified in the conventional way by an integrated hearing aid. The two systems – acoustic and electrical hearing – are programmed to blend together. The hearing centres of the brain learn to merge the signals, restoring sound perception across the entire pitch range to the user.
Auditory brainstem implant (ABI)
Only a few centres in the UK offer this highly specialist hearing implant, designed for patients who have damage to the hearing nerve through disease or developmental anomaly. Patients requiring this type of implant are unable to benefit from any other type of hearing technology. ABI surgery is highly complex and is often part of a much longer operation on the brainstem. The ABI is an electrode pad that is placed on the hearing centre of the brainstem itself, called the cochlear nucleus. The electrical signals from the ABI stimulate the hearing cells in the cochlear nucleus that then trigger the auditory pathway up to the hearing centres in the brain.
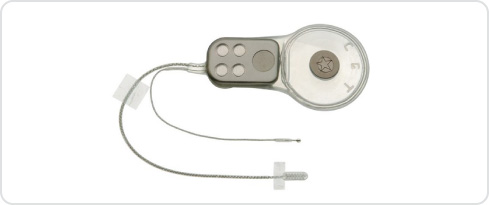
The patient returns for switch-on 6-8 weeks after surgery. The outcome is much less predictable than with a cochlear implant. However some patients do regain useful hearing from an ABI that helps with lip-reading and communication.
Related pages

Getting here
Information about travelling to, staying at and getting around the hospital.

Jobs at UHB
A great place to work. Learn why.


